Electronic private prescribing is rapidly replacing paper-based systems across UK pharmacies and clinics. As the demand for private healthcare services grows — from weight management and travel health to sexual health and aesthetic treatments — pharmacists and prescribers need efficient, compliant digital workflows. This complete guide explains what electronic private prescribing is, how it works, who can do it, and how to get started.
What Is Electronic Private Prescribing?
Electronic private prescribing is the process of generating, managing, and issuing private prescriptions digitally rather than on paper. Instead of handwriting prescriptions on FP10P forms, prescribers use private prescription software to create legally valid electronic prescriptions complete with patient details, medication information, dosage instructions, and prescriber signatures.
An electronic private prescription contains the same legal information as a paper prescription — patient name and address, date, medication details, prescriber signature and registration number — but is generated, stored, and transmitted digitally. This creates automatic audit trails, reduces errors, and enables faster dispensing.
How Does Electronic Private Prescribing Work?
The typical electronic private prescribing workflow follows these steps:
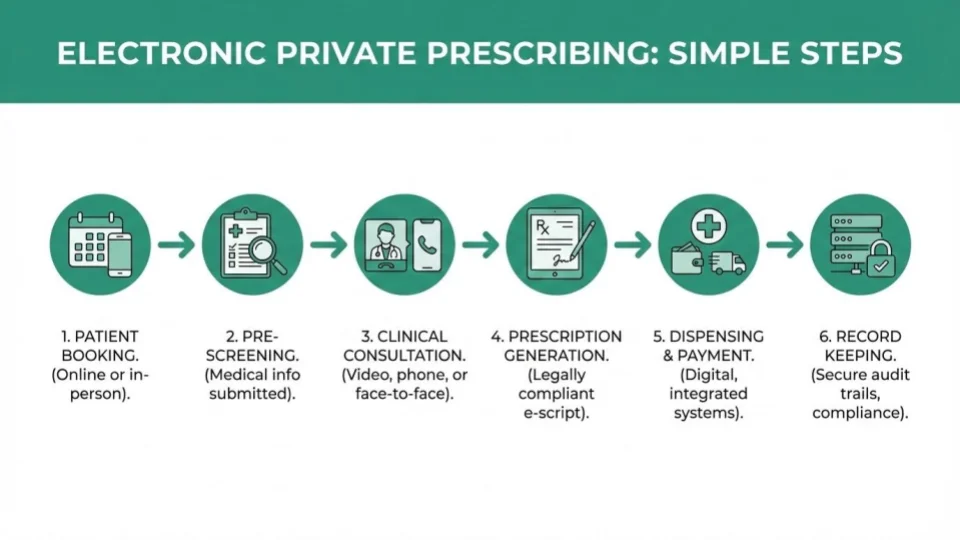
Step 1: Patient Booking
Patients book a consultation online or in person. Modern platforms include integrated booking systems that capture patient details, medical history, and the reason for consultation before the appointment.
Step 2: Pre-Screening
Before the consultation, patients complete pre-screening questionnaires. These flag potential contraindications, allergies, and relevant medical history — ensuring the prescriber has critical safety information before the appointment begins.
Step 3: Clinical Consultation
The prescriber conducts a clinical consultation — face-to-face, telephone, or video. With pharmacy consultation software, this consultation follows SmPC-guided templates that embed safety checks, dosage guidance, and contraindication warnings directly into the workflow.
Step 4: Prescription Generation
If clinically appropriate, the prescriber generates an electronic private prescription within the software. The prescription includes all legally required fields: patient details, medication (name, form, strength, quantity), directions, prescriber details, and date. The prescription is digitally signed.
Step 5: Dispensing & Payment
The prescription is dispensed (either on-site or sent to a dispensing pharmacy) and payment is processed. Integrated platforms handle payment processing alongside prescribing, eliminating the need for separate payment systems.
Step 6: Record Keeping
Every step is automatically logged — creating a complete audit trail from booking through dispensing. This is essential for GPhC and CQC compliance inspections.
Who Can Issue Private Prescriptions Electronically?
In the UK, the following registered professionals can issue private prescriptions:
- Doctors (GMC registered) — Can prescribe any medication within their competence
- Independent Prescriber Pharmacists (GPhC registered) — Can prescribe any medication within their competence since 2026 legislative changes
- Dentists (GDC registered) — Can prescribe within dental practice scope
- Nurse Independent Prescribers (NMC registered) — Can prescribe from the full formulary
- Supplementary Prescribers — Can prescribe within an agreed Clinical Management Plan
Pharmacist independent prescribers represent the fastest-growing group of private prescribers in the UK, driven by expanded prescribing rights and the growth of pharmacy-led private services.
Benefits of Electronic vs Paper Private Prescribing
Switching from paper to electronic private prescribing delivers measurable improvements across safety, efficiency, and compliance:
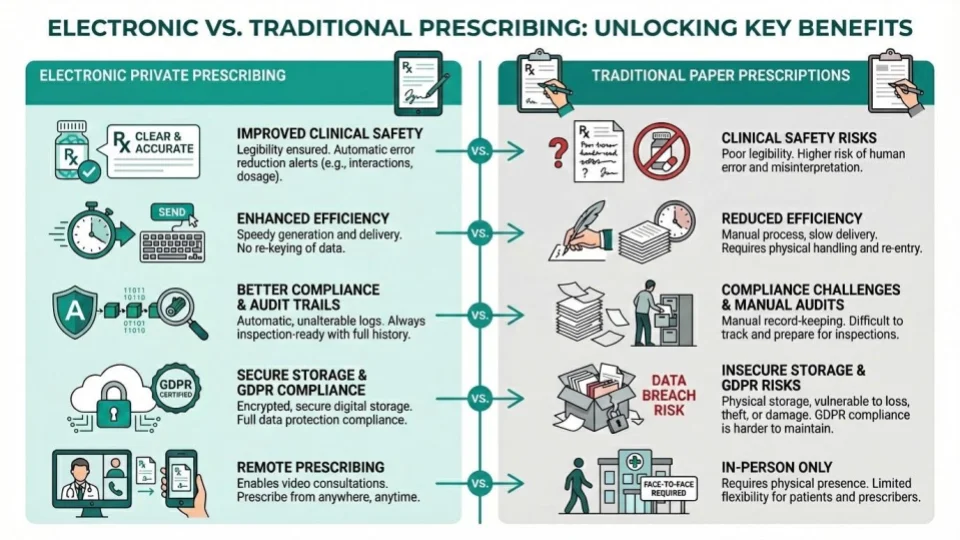
Clinical Safety
- Legibility: Eliminates handwriting errors — the most common cause of dispensing errors
- Built-in checks: Software can flag contraindications, interactions, and dosage errors
- SmPC guidance: Clinical consultation templates embed safety information at the point of prescribing
- Standardised workflows: Every consultation follows the same structured, evidence-based process
Efficiency
- Speed: Electronic prescriptions are generated in seconds, not minutes
- No re-keying: Patient details auto-populate from records
- Integrated payments: No separate payment processing step
- Remote prescribing: Video consultations enable prescribing without physical presence
Compliance & Audit
- Automatic audit trail: Every action is timestamped and logged
- Inspection-ready records: GPhC and CQC inspectors can review digital records instantly
- Secure storage: Electronic records are backed up and encrypted, unlike paper files
- GDPR compliance: Digital systems enable proper data access controls and retention policies
Legal Requirements for Electronic Private Prescriptions in the UK
Electronic private prescriptions must meet the same legal requirements as paper prescriptions. The key regulations include:
The Human Medicines Regulations 2012
All private prescriptions must include: prescriber name, address, and professional registration number; patient name and address; date; medication details (name, form, strength, quantity, directions); and prescriber signature.
GPhC Standards
The General Pharmaceutical Council requires pharmacies to maintain adequate records of all prescriptions dispensed, ensure patient safety through appropriate clinical checks, and maintain confidentiality of patient information.
CQC Requirements (for clinics)
The Care Quality Commission requires registered providers to maintain complete patient records, demonstrate clinical governance, and ensure safe prescribing practices.
GDPR / UK Data Protection Act 2018
All patient data must be processed lawfully, stored securely, retained only as long as necessary, and accessible to patients on request. Electronic systems must implement appropriate technical and organisational security measures.
How to Get Started with Electronic Private Prescribing
Setting up electronic private prescribing in your pharmacy or clinic involves four key steps:
- Choose your software: Select a platform that covers your needs — from basic prescription generation to full patient journey management including booking, consultations, and payments. See our comparison of the best private prescription software for UK pharmacies.
- Set up your services: Configure the private services you’ll offer (weight management, travel health, sexual health, etc.) with appropriate consultation templates and pricing.
- Train your team: Ensure all prescribers and support staff understand the software workflow, clinical governance requirements, and compliance procedures.
- Launch and promote: Make your private services visible to patients through your website, social media, and in-pharmacy marketing.
Choosing the Right E-Prescribing Software
Not all e-prescribing software is the same. When evaluating platforms, consider:
- Scope: Does it only generate prescriptions, or does it cover the full patient journey (booking, consultations, payments)?
- Clinical safety: Does it include SmPC-guided consultation templates with built-in safety checks?
- Compliance: Does it provide GPhC/CQC-ready audit trails and compliance dashboards?
- Pricing model: Flat monthly fee vs per-prescription charges — which is more cost-effective at your volume?
- Scalability: Can it support multiple sites if you expand?
RxSure covers the complete workflow — from online booking through SmPC-guided consultations, electronic prescription generation, integrated payments, and compliance management — for a flat monthly fee with no per-prescription charges.
The Future of Electronic Private Prescribing
Electronic private prescribing is set to become the standard across UK pharmacy and clinic settings. Key trends driving adoption include:
- Expanded pharmacist prescribing rights enabling more pharmacy-led services
- Patient expectation for digital-first healthcare experiences
- Regulatory pressure for better record-keeping and clinical governance
- AI-assisted clinical support embedded in prescribing workflows
- Integration with NHS services through initiatives like Pharmacy First
Pharmacies and clinics that adopt electronic private prescribing will position themselves better to grow their private services, meet compliance requirements, and deliver the patient experience modern healthcare demands.
Key Takeaways
- Electronic private prescribing replaces paper with digital workflows — improving safety, speed, and compliance
- Pharmacist independent prescribers are the fastest-growing group of private prescribers in the UK
- Legal requirements are the same for electronic and paper prescriptions
- The best platforms cover the complete patient journey, not just prescription generation
- SmPC-guided consultation templates are the gold standard for clinical safety
- Automatic audit trails make GPhC and CQC inspections simpler




